Are you GingerSteady?
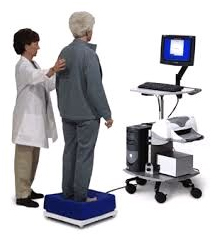
The goal of our GingerSteady balance program is specially designed to reduce loss of balance in the older adult. Problems include dizziness or loss of balance associated with vestibular dysfunction, joint stiffness, muscle weakness or due to an individual's lack of physical activity.
We also specialize in treating patients with balance impairment related to neurological deficits such as stroke , Parkinson's Disease, Spinal Cord Injury, Brain Injury or other traumatic injuries to increase balance , movement and educate the patient and caregiver of compensatory strategies needed to be independent.
If you're feeling unsteady, dizzy, lightheaded, had periods of loss of balance, had or have been told you have Vertigo, had a previous fall or you just feel that your balance is a little off, you need to see a physical therapist >> us.
Red Flags
How we can help
Falls
Fear of Falling
Common locations of falls
Common time of falls
Prevention Tips: Medications/ Vision/ Nutrition
Home Safety/ Home Assessment and Modification
Vestibular Disorders and Rehabilitation
References
Schedule your appointment at
813-631-9700
We are here to help!
Red flags which put you at risk for balance and falls:
- Have you had any falls in the last six months?
- Do you take four or more prescription or over-the-counter medications daily?
- Do you have any difficulty walking or standing?
- Do you use a cane, walker, or crutches, or have to hold onto things when you walk?
- Do you have to use your arms to be able to stand up from a chair?
- Do you ever feel unsteady on your feet, weak, or dizzy?
- Has it been more than two years since you had an eye exam?
- Has your hearing gotten worse with age, or do your family or friends say you have a hearing problem?
- Do you usually exercise less than two days a week? (for 30 minutes total each of the days you exercise) Do you drink any alcohol daily?
- Do you have more than three chronic health conditions? (such as heart or lung problems, diabetes, high blood pressure, arthritis, etc. Ask your doctor(s) if you are unsure.)
If you answered "yes" to 2 or more of these questions, you may be at risk.
Reference:
National Center for Injury Prevention and Control. Preventing Falls: How to Develop Community-based Fall Prevention Programs for Older Adults. Atlanta, GA: Centers for Disease Control and Prevention, 2008.

We can help reduce falls risk:
- Improve Balance and Vestibular Function
- Evidence-based Outcomes
- Improve muscle function, joint movements, proprioceptive sensations
- Evaluation & Home Modification to Improve Safety
- Educate Individual and Family to Reduce Falls
- Promote Safe and Independent Living
- Reduce Need for Urgent Care
- Reduce Hospitalization Recurrence
Improve YOUR Quality of Life!
During the initial evaluation, the Doctor of Physical Therapy will do a comprehensive examination. This will include a review of your medical history including medications you're taking, asking you questions about the onset of symptoms, what makes it worse, what makes it better, and complete a series of tests. This will help the therapist create an individualized plan of treatment that fits your needs. The therapist will work with you on exercises to reduce your dizziness, improve your balance and muscle strength leading to an improved functional mobility. The therapist will also provide education and training to your caregiver(s) to ensure that you are able to practice these exercises at home.
Move Forward-American Physical Therapy Association (2016)
Reduce your risk of falls- Our physical therapist will assess hazards in your home and recommend changes as needed.
Reduce your fear of falling- We will help you regain your confidence so that you can move freely without the fear of falling.
Improve Mobility- We will establish an individualized treatment plan that will allow you to increase your strength and skills in movement.
Improve your balance and strength- We will train you balance exercises that address specific muscles needed to improve your overall balance and strength.
Improve movement, flexibility and posture- Treatments will help restore normal movements from joint stiffness. Instructions will be given to improve flexibility and posture.
Falls
- Not a normal part of aging (National Council on Aging (NCOA), 2014)
- A major global health problem (World Health Organization (WHO), 2014)
- The second leading cause of accidental injury or deaths worldwide (WHO, 2014)
- Fall rates increase with age (Currie, 2008)
- Age alone does not identify older adults most likely to fall (Wu, Yang, Kuo, Wong, and Liaw, 2013)
- A third to three quarters of falls in older adults occur at home (Gopaul and Connely, 2012)
- 33% of those aged 65 years and older fall each year (Centers for Disease Control and Prevention (CDC), 2013)
- Falls affect 50% of older adults over the age of 80 (Ambrose, Paul, and Hausdorff, 20 13)
- 37.7 million falls worldwide are severe enough to require medical attention (WHO, 2014)
Fear of Falling
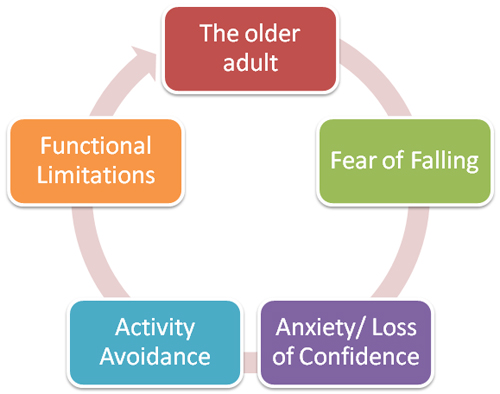
(Stenhagen, Ekstrom, Nordell, and Elmstahl, 2014)
Common Location of Falls
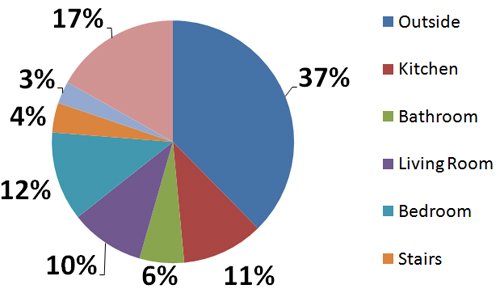
(Elliot, Painter, and Hudson, 2009)
Common Time of Falls
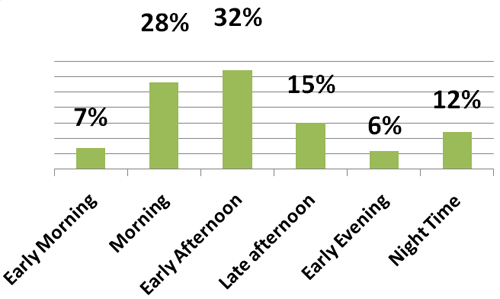
(Elliot, Painter, and Hudson, 2009)
Prevention Tips
Talk to your physician, review your medications:
- Polypharmacy- the use of multiple medications due to health issues
- Average of 2-6 prescribed medications and 1 to 3.4 non-prescribed medications
- 66% of older adults use one or more drugs daily
(Heuberger and Caudell, 2011) - Highest risk of falls are associated with psychotropic medications
(The American Geriatrics Society, 2014)
![]()
Get a vision exam:
- Impaired vision leads to misjudgment of distance and spatial information
(Ambrose, Paul, and Hausdorff, 20 13) - Individuals with visual impairment are 7x more likely to have a fall
(Newton and Sanderson, 2013) - Persons who wear multifocal lenses are 2x more likely to fall (Al- Aama, 2011)
- Have a vision exam once a year (NCOA, 2014)
Nutrition:
- Nutrition risk precedes malnutrition (Watson, Zhang, & Wilkinson, 2010)
- Age related loss of muscle mass is associated with undernutrition (Stoltz et al., 2002)
- Prevalence of undernutrition in older adults is around 20 to 60% (Stoltz et al., 2002)
- Elevated body mass index of 30 kg/m2 is associated with increased tendency of falls (Stoltz et al., 2002)
Home Assessment and Modification
- 60% of falls happen at home (National Institute of Health SeniorHealth, 2013)
- Home assessment results in 21% reduction in falls (Pighills, Torgerson, Sheldon, Drummond, & Bland, 2011)
- Interior and exterior of the home needs to assessed for environmental fall risk factors (Elliot, Painter, & Hudson, 2009)
- Home hazard identification and management by a physical or occupational therapist (Pighills, Torgerson, Sheldon, Drummond, & Bland, 2011)
Steps for Home Safety (Centers for Disease Control and Prevention, 2016)
- Remove things you can trip over (such as papers, books, clothes, and shoes) from stairs and places where you walk.
- Install handrails and lights on all staircases.
- Remove small throw rugs or use double-sided tape to keep the rugs from slipping.
- Keep items you use often in cabinets you can reach easily without using a step stool.
- Put grab bars inside and next to the tub or shower and next to your toilet.
- Use non-slip mats in the bathtub and on shower floors.
- Improve the lighting in your home. As you get older, you need brighter lights to see well. Hang lightweight curtains or shades to reduce glare.
- Wear shoes both inside and outside the house. Avoid going barefoot or wearing slippers.
Vestibular Disorders and Rehabilitation
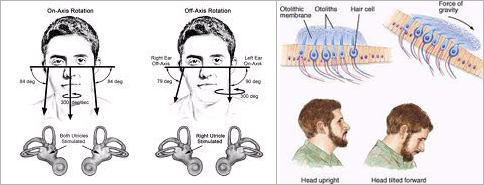
Vertigo is a type of dizziness that causes the person to experience a sensation of motion, it is the most common complaint by patients when the vestibular system is involved. This can result from a fall, stroke, brain injury or other traumatic injuries or diseases as well as from dysfunctions within the vestibular system such as Benign Paroxysmal Positional Vertigo (BPPV), peripheral vestibular dysfunction, vestibular neuritis, acoustic neuroma and migraine associated dizziness, among others. Symptoms may include the feeling of tilting, spinning or swaying and can last for a few seconds to days in some individuals.
Vestibular disorders are usually not life threatening but can result in significant disability, thus resulting in the decrease of an individual's quality of life. It is important to first see your physician to determine the cause of your symptoms to rule out more serious medical conditions.
Our Vestibular Rehabilitation program is designed to diminish/ reduce symptoms of dizziness or loss of balance.Treatment includes risk reduction for falling or loss of balance, canalith repositioning maneuver by your physical therapist, exercises to strengthen your systems of balance and instructions on compensatory strategies that will help you adapt to improve your quality of life.
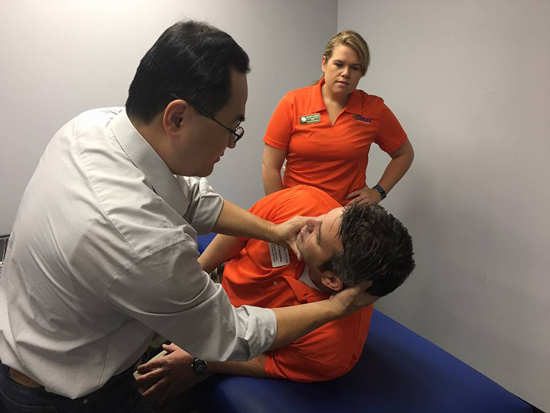
Benign Paroxysmal Positional Vertigo (BPPV)(Goodman & Fuller, 2009)
- A mechanical disorder of the inner ear
- Characterized by episodes of vertigo with changes in head position
- May wake up dizzy after changes in position at night time.
- Represents ~20-40% of peripheral vestibular problems
- 20% involves more than one canal
Vestibular Neuritis (Goodman & Fuller, 2009)
- Second most common cause for vertigo
- Often caused by a viral infection
- No cochlear involvement (hearing usually spared)
- Head movement cause blurred vision
- Perception of rotation (to the involved side when eyes are closed and opposite side when eyes are open)
Endolymphatic Hydrops (Goodman & Fuller, 2009)
- Menier's syndrome is the most common form
- Episodes of vertigo due to pressure changes within the closed fluid system causing vestibular and cochlear dysfunction
- Initial fullness of the ear , a reduction of hearing and Tinnitus (ringing of ears). This is followed by rotational vertigo, imbalance in posture, nystagmus and nausea.
- Can last from hours to days
Perilymph Fistula (Goodman & Fuller, 2009)
- Vertigo caused by abnormal communication of the middle and inner ear spaces
- May result from congenital malformations, pressure applied to external ear or from prior ear surgery
- Symptoms decreased with rest and increases with activity
- Symptoms may also increase with the Valsalva maneuver (forcibly exhaling while keeping nose and mouth closed)
- Fistula may be caused by heavy lifting, sneezing, head trauma or overaggressive exercise.
Additional Reading on Evaluating Tools for Vestibular Imbalance
References
Al-Aama, T. (2011).Falls in the Elderly: spectrum and prevention. Canadian Family Physician, 57(7), 771-776. Retrieved from http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3135440/
Ambrose, A., Paul, G., & Hausdorff, J. (2013). Risk factors for falls among older adults: a review of literature. Maturitas, 75(1), 51-61. doi:10.1016/j.maturitas.2013.02.009
Centers for Disease Control and Prevention. (2013). Falls among older adults: an overview. Retrieved March 30, 2014, from http://www.cdc.gov/homeandrecreationalsafety/falls/adultfalls.html
Centers for Disease Control and Prevention. (2016, March 30). Preventing Falls Among Older Adults. Retrieved March 30, 2016, from http://www.cdc.gov/Features/OlderAmericans/
Currie, L. (2008).Fall and Injury Prevention. In R. Hughes (Ed.), Patient safety and quality: an evidence-based handbook for nurses (pp. 203-258). Rockville, MD: AHRQ Publication. Retrieved from http://www.ahrq.gov/professionals/clinicians-providers/resources/nursing/resources/nurseshdbk/nurseshdbk.pdf
Elliot, S., Painter, J., & Hudson, S. (2009). Living alone and fall ris factors in community-dwelling middle age and older adults. Journal of Community Health, 34(4), 301-310. doi:10.1007/s10900-009-9152-x
Goodman, C., & Fuller, K. (2009).PATHOLOGY Implications for the Physical Therapist (3rd ed.). St. Louis, Missouri: Saunders Elsevier.
Gopaul, K., & Connely, D. (2012). Fall risk beliefs and behaviors following a fall in community-dwelling older adults: a pilot study. Physical and Occupational Therapy in Geriatrics, 30(1), 53-72. doi:10.3109/02703181.2011.649230
Heuberger, R., & Caudell, K. (2011). Polypharmacy and nutritional status in older adults: a cross-sectional study. Drugs Aging, 28(4), 315-323.doi:10.2165/11587670-000000000-00000
Hull, W., & Newell, L. (2008). Balanced for Life.
Move Forward-American Physical Therapy Association. (2016, March 30). Retrieved March 30, 2016, from http://www.moveforwardpt.com/symptomsconditionsdetail.aspx?cid=1bb9c784-a874-43b1-976f-d0de03c19f99
National Council on Aging. (2014). Debunking the Myths of Older Adult Falls. Retrieved April 5, 2014, from http://www.ncoa.org/improve-health/falls-prevention/debunking-the-myths-of-older.html
National Council on Aging. (2014). Falls prevention: fact sheet. Retrieved March 31, 2016, from http://www.ncoa.org/press-room/fact-sheets/falls-prevention-fact-sheet.html
National Institute of Health SeniorHealth.(2013). Fall Proofing Your Home. Retrieved April 13, 2014, from http://nihseniorhealth.gov/falls/homesafety/01.html
Newton, M., & Sanderson, A. (2013).The effect of visual impairment on patients fall risk. Nursing Older People, 25(8), 16-21. doi:10.7748/nop2013.10.25.8.16.e489
Pighills, A., Torgerson, D., Sheldon, T., Drummond, A., & Bland, J. (2011). Environmental assessment and modification to prevent falls in older people. Journal of the American Geriatric Society, 59(1), 26-33. doi:10.1111/j.1532-5415.2010.03221.x.
Stenhagen, M., Ekstrom, H., Nordell, E., & Elmstahl, S. (2014). Accidental falls, health-related quality of life and life satisfaction: a prospective study of the general elderly population. Archives of Gerontology and Geriatrics, 58(1), 95-100. doi:10.1016/j.archger.2013.07.006
Stoltz, D., Miller, M., Bannerman, E., Whitehead, C., Crotty, M., & Daniels, L. (2002).Nutrition screening and assessment of patients attending a multidisciplinary falls clinic. Nutrition and Dietetics, 59(4), 234-239. Retrieved from http://www.thefreelibrary.com/Nutrition+screening+and+assessment+ of+patients+attending+a...-a096810648
Watson, S., Zhang, Z., & Wilkinson, T. (2010). Nutritional risk screening in community-living older people attending medical or falls prevention services. Nutrition and Dietetics, 67(2), 84-89. doi:10.1111/j.1747-0080.2010.01424.x
World Health Organization.(2012). Interesting facts about ageing. Retrieved March 31, 2016, from http://www.who.int/ageing/about/facts/en/
World Health Organization.(2014). Falls. Retrieved March 31, 2016, from http://www.who.int/mediacentre/factsheets/fs344/en/
Wu, T., Yang, R., Kuo, K., Wong, W., &Liaw, C. (2013).Risj factor for single or recurrent falls: a prospective study of falls in community dwelling seniors without cognitive impairment. Preventive Medicine, 511-517. doi:10.1016/j.ypmed.2013.07.012
National Center for Injury Prevention and Control. Preventing Falls: How to Develop
Fall Prevention Programs for Older Adults. Atlanta, GA: Centers for Disease Control and Prevention, 2008.








